Spotting: What’s Normal, What’s Not
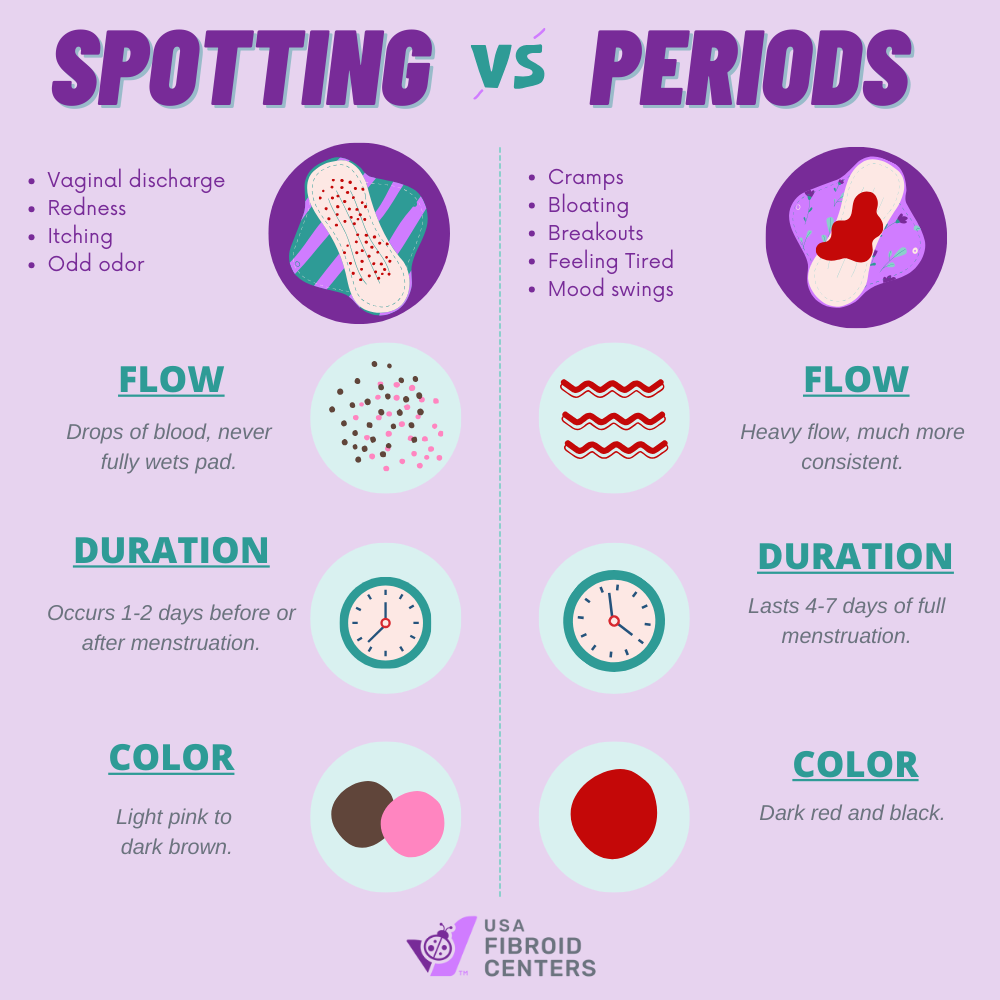
Spotting is light bleeding that occurs outside of your regular menstrual period. It’s typically lighter than a normal flow, more like a stain than soaking a pad. The color can range from bright red to dark brown and may appear suddenly or last a few days. Many people experience spotting at some point.
Defining 'normal' for menstrual cycles is difficult due to natural variation. Cycles typically range from 21 to 35 days, and anything within this range can be healthy. Spotting can occur within this range, particularly with longer cycles. However, any change in your usual pattern warrants attention.
Spotting isn't always a reason to panic, but it shouldn't be automatically dismissed. Understanding your body and health is key. Recognizing what’s typical for you is the first step.
Hormonal Shifts and Spotting
Hormones, primarily estrogen and progesterone, orchestrate the menstrual cycle. Fluctuations in these hormones can cause spotting. Estrogen levels rise and fall, affecting the uterine lining's stability. When estrogen dips, it can lead to shedding before a period is due.
Ovulation, the release of an egg, can also cause spotting due to a slight dip in estrogen. The luteal phase, between ovulation and your period, is governed by progesterone. Insufficient progesterone can lead to spotting during this phase.
Perimenopause, the transition to menopause, involves significant hormonal changes. Erratic estrogen levels can lead to increased spotting, often an early sign. Hormonal birth control methods also affect spotting. Combined pills usually regulate cycles but can cause initial spotting. Progestin-only methods, such as some IUDs and implants, can also cause irregular bleeding, especially early on.
Common Causes Beyond Hormones
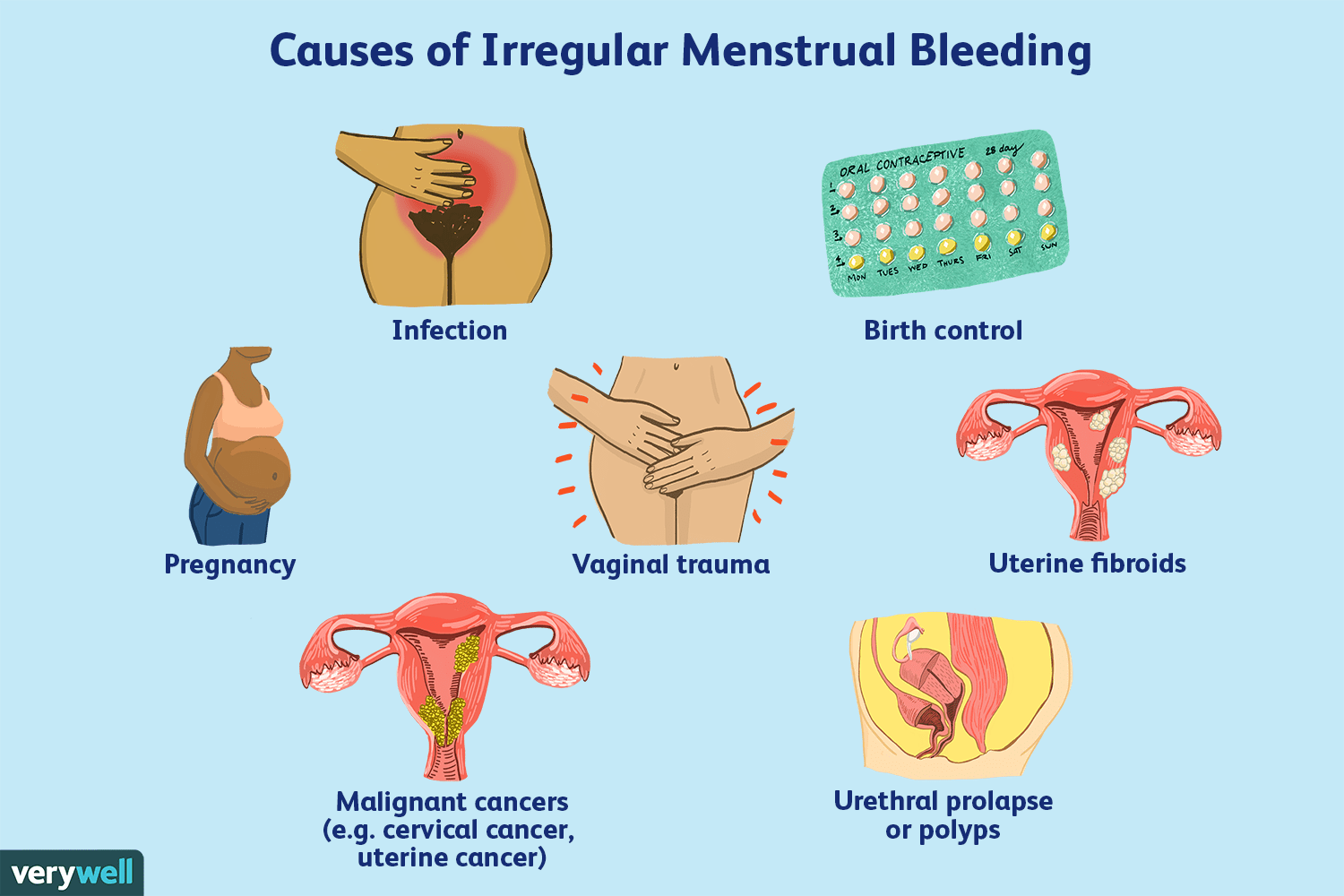
While hormones are a frequent cause, spotting can signal other issues. Infections like STIs (chlamydia, gonorrhea), yeast infections, or bacterial vaginosis can cause inflammation and bleeding, though spotting isn't always the primary symptom.
Structural abnormalities in the uterus can cause spotting. Polyps (benign growths), fibroids (non-cancerous tumors), endometriosis (uterine tissue outside the uterus), and adenomyosis (uterine tissue within the uterine wall) can lead to irregular bleeding, often with painful periods.
It's crucial to remember I am not a medical professional and cannot diagnose any condition. If you’re experiencing spotting, especially if it's accompanied by other symptoms like pelvic pain, fever, or unusual discharge, it's important to seek medical attention. These conditions frequently present with other symptoms alongside spotting, offering clues to what might be happening.
Less frequently, spotting could be related to changes in the cervix, but this is usually investigated when other causes have been ruled out. It's a complex picture, and a proper diagnosis requires a thorough evaluation by a healthcare provider.
Spotting and Your Contraception
Spotting is common with contraception, particularly when starting a new method. Combined pills (estrogen and progestin) can cause spotting for the first three to six months during adjustment. Progestin-only pills ('mini-pills') are more likely to cause irregular bleeding and spotting than combined pills.
Hormonal IUDs release progestin and commonly cause spotting in the first few months, usually subsiding within a year. Copper IUDs can lead to heavier periods and occasional spotting. Implants also release progestin and can cause unpredictable bleeding.
The contraceptive shot is known for causing irregular bleeding. Distinguish between 'breakthrough bleeding' (heavier, period-like) and true spotting. If spotting persists or is accompanied by other symptoms, consult your doctor.
Contraceptive Methods and Spotting
| Method | Spotting Likelihood | Typical Duration | Possible Reasons |
|---|---|---|---|
| Combined Oral Contraceptive Pills | Medium | First 3 months, or with missed pills | Hormonal adjustment, inconsistent use |
| Progestin-Only Pills | Medium | Irregular throughout use | Hormonal fluctuations, lower estrogen levels |
| Hormonal IUD | High initially, then Low | First 3-6 months | Body adjusting to the IUD, uterine irritation |
| Copper IUD | Medium to High | Often heavier and longer than hormonal spotting | Uterine irritation, increased inflammation |
| Contraceptive Patch | Medium | First few months, or with improper application | Hormonal adjustment, adhesive issues |
| Vaginal Ring | Medium | First month, or with expulsion/slippage | Hormonal adjustment, inconsistent release |
| Depo-Provera Injection | High initially, then Low | First 3-6 months | Progestin-only, significant hormonal shift |
| Implant | Medium to High | First 6-12 months | Progestin-only, body adjusting to continuous hormone release |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
When to See a Doctor
Knowing when spotting warrants a visit to the doctor is vital. While occasional, light spotting is often harmless, certain symptoms should always prompt medical attention. Heavy spotting, defined as soaking through a pad or tampon every hour for several hours, is a clear red flag. Spotting accompanied by severe pelvic pain, fever, dizziness, or fainting spells needs immediate evaluation.
Spotting after menopause – meaning after you've gone 12 consecutive months without a period – is never normal and requires investigation. A sudden change in your spotting pattern, such as a significant increase in frequency or duration, is also a reason to see a doctor. Don't ignore persistent spotting that doesn't improve after a few months.
During a doctor's visit, you can expect a pelvic exam to assess your reproductive organs. An ultrasound may be ordered to visualize your uterus and ovaries. Blood tests can check your hormone levels, rule out pregnancy, and look for signs of infection or anemia. The doctor will consider your medical history and symptoms to determine the best course of action.
I want to emphasize that seeking medical advice isn’t about overreacting; it’s about being proactive about your health. Early diagnosis and treatment can prevent complications and improve your overall well-being.
Spotting and Fertility
The link between spotting and fertility is complex. Spotting can sometimes indicate implantation bleeding, which occurs when a fertilized egg attaches to the uterine lining. Implantation spotting is typically lighter and shorter than other types of spotting.
Spotting can disrupt ovulation, making conception harder. Irregular cycles and unpredictable bleeding complicate pinpointing your fertile window. If trying to conceive and experiencing frequent spotting, track your cycle and consult a fertility specialist.
For those undergoing fertility treatments, spotting can cause anxiety. Communicate any spotting to your doctor, as it may indicate a complication. Spotting doesn't necessarily mean a pregnancy isn't viable, but it warrants investigation. Seeking support is important.
Managing Spotting: Practical Tips
undefined, though they may require more frequent emptying.
Tracking your cycle is essential for identifying patterns and understanding what might be causing your spotting. There are many apps available for cycle tracking, or you can use a traditional calendar. Paying attention to lifestyle factors like stress, diet, and exercise can also be helpful. High stress levels can disrupt hormone balance and contribute to spotting.
Prioritizing self-care and maintaining a healthy lifestyle can positively impact your overall menstrual health. Periuod offers a range of products designed to make your period more comfortable and manageable, from pads to menstrual cups. Remember, taking care of your body is an investment in your well-being.
Recent Research & Emerging Insights (2026)
Research into the causes of irregular bleeding and spotting is ongoing. Recent studies are exploring the role of the microbiome in menstrual health and the potential for targeted therapies to regulate hormone imbalances. New diagnostic tools, such as advanced ultrasound techniques, are improving our ability to identify structural abnormalities in the uterus.
At Periuod, we're committed to staying at the forefront of menstrual health research and providing you with the most up-to-date information. Our understanding of spotting and irregular bleeding is constantly evolving, and we'll continue to share new insights as they become available.





No comments yet. Be the first to share your thoughts!