Why Your Period Hurts: Beyond ‘Just Cramps’
For many, "period cramps" feels like a dismissive term for what can be genuinely debilitating pain. It's more than just a little discomfort; it’s a complex physiological process. The primary culprit is prostaglandins, hormone-like substances that trigger uterine contractions to shed the uterine lining. These contractions restrict blood flow to the muscles, causing pain. But why does the intensity vary so much?
The amount of prostaglandins your body produces significantly impacts pain levels. Higher levels generally mean stronger contractions and more intense cramps. Inflammation also plays a role, contributing to the overall discomfort. It’s easy to fall into the trap of thinking some pain is "normal,’ but that"s a dangerous mindset. While some mild discomfort is common, pain that disrupts your daily life is not something you should simply endure.
It's important to be aware that what feels like 'cramps' might actually be something else. Conditions like endometriosis, where uterine tissue grows outside the uterus, or fibroids, noncancerous growths in the uterus, can cause period-like pain, often more severe. According to MedlinePlus, endometriosis can cause chronic pelvic pain, and fibroids can lead to heavy bleeding and discomfort (MedlinePlus, Period Pain, 2024). I'm not suggesting self-diagnosis, but recognizing these possibilities is key to seeking appropriate care when needed.

Heat: Your First Line of Defense
Heat is often the first thing people reach for when cramps strike, and for good reason. It works on multiple levels. Applying heat to the lower abdomen helps relax the uterine muscles, reducing the intensity of contractions. This relaxation also increases blood flow to the area, delivering oxygen and nutrients that can ease discomfort. There’s also evidence suggesting heat may reduce prostaglandin production, tackling the problem at its source.
You have options when it comes to applying heat. Traditional heating pads are effective, but hot water bottles can be a comforting alternative. Warm baths, especially with Epsom salts, provide all-over relaxation. Adhesive heat patches are convenient for on-the-go relief. However, safety is crucial. The Mayo Clinic recommends using a low to medium heat setting and limiting application to 20 minutes at a time to avoid burns (Mayo Clinic, Menstrual cramps, 2024).
Beyond the physical benefits, heat offers psychological comfort. The warmth can be incredibly soothing, providing a sense of calm and well-being during a potentially stressful time. It’s a simple, accessible, and often incredibly effective method for managing period pain.
Movement: Gentle Exercise for Pain Relief
The idea of exercising when you're cramping might seem counterintuitive, but gentle movement can actually be incredibly beneficial. Low-impact exercises like walking, yoga, and stretching release endorphins, your body’s natural pain relievers. These endorphins can help block pain signals and improve your overall mood. Movement also improves circulation, which can reduce muscle tension and alleviate cramps.
Specific yoga poses are particularly helpful. Child’s pose gently stretches the lower back and abdomen, relieving tension. Cat-cow pose improves spinal mobility and can ease cramping. You can find detailed instructions for these poses online – a quick search for "yoga for menstrual cramps’ will yield numerous resources. Remember, the goal isn"t a strenuous workout, but gentle, restorative movement.
It’s vital to listen to your body. If something feels painful, stop. Don’t push yourself beyond your limits. This is about finding gentle ways to ease discomfort, not adding to it. Even a short, slow walk can make a difference.
Dietary Shifts: Foods That Fight Inflammation
Inflammation is a key player in period pain, so adjusting your diet to reduce inflammation can be a powerful strategy. It's not about restrictive dieting, but about making conscious food choices. Focus on incorporating foods rich in omega-3 fatty acids, like salmon, flaxseeds, and chia seeds. These fats have anti-inflammatory properties that can help reduce cramping.
Magnesium is another important nutrient. Leafy green vegetables, dark chocolate (yes, really!), and nuts are good sources. Fiber-rich foods, such as fruits, vegetables, and whole grains, also contribute to overall health and can help regulate your cycle. NCBI’s InformedHealth.org notes that a balanced diet supports overall well-being during menstruation (NCBI, Overview: Period pain, 2023).
Conversely, limiting certain foods can also help. Processed foods, sugary drinks, and excessive caffeine can all contribute to inflammation. While a cup of coffee might seem appealing when you're feeling sluggish, it can actually worsen cramps for some people. I'm hesitant to recommend a specific diet like the Mediterranean diet as a guaranteed solution, as the evidence isn’t conclusive enough, but adopting its principles of whole, unprocessed foods is generally a good idea.
Food Choices & Potential Impact on Menstrual Cramps
| Food Item | Inflammation Level | Potential Benefits | Potential Drawbacks |
|---|---|---|---|
| Spinach | Low | Rich in iron, which can combat fatigue often experienced during menstruation. Contains magnesium, potentially easing muscle tension. | May cause bloating in some individuals if consumed in very large quantities. |
| Salmon | Low | Excellent source of omega-3 fatty acids, known for their anti-inflammatory properties which may reduce cramp severity. | Can be relatively expensive compared to other protein sources. |
| Ginger | Low | Contains gingerol, a natural anti-inflammatory compound. May help reduce prostaglandin production, lessening uterine contractions. | May interact with blood-thinning medications; consult a healthcare professional if you are taking such medication. |
| Dark Chocolate (70% cacao or higher) | Low to Medium | Contains magnesium and antioxidants. May improve mood and reduce stress, which can exacerbate pain perception. | High sugar content in some varieties can lead to energy crashes and potentially worsen inflammation if consumed excessively. |
| Coffee | Medium to High | May provide a temporary energy boost, potentially alleviating fatigue. | Can worsen anxiety and potentially increase inflammation in some people. Caffeine can also contribute to dehydration, which may worsen cramps. |
| Pizza | High | Can be a source of comfort food and temporary satisfaction. | Typically high in unhealthy fats, salt, and processed ingredients, which can promote inflammation and worsen cramps. Often leads to bloating. |
| Bananas | Low | Good source of potassium, an electrolyte that can help reduce muscle cramps and bloating. | May cause digestive issues in some people if consumed in excess. |
| Turmeric | Low | Contains curcumin, a potent anti-inflammatory compound. May help reduce pain and inflammation throughout the body. | Bioavailability can be low; consuming with black pepper can enhance absorption. |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
Supplements: What the Research Says
Supplements are often touted as period pain relief, but it’s important to approach them with caution and a critical eye. Magnesium is frequently recommended, and some studies suggest it can help reduce cramping. MedlinePlus notes that magnesium deficiency can worsen PMS symptoms (MedlinePlus, Magnesium, 2023). Dosages vary, but 200-400mg per day is a common range, but always check with your doctor.
Vitamin D, particularly if you’re deficient, may also play a role. Vitamin E has shown some promise in reducing pain, and fish oil, rich in omega-3 fatty acids, can help combat inflammation. However, the research is often mixed and dosages need to be carefully considered. It's crucial to remember that 'may help' is very different from 'is proven to cure'.
Before starting any new supplement regimen, talk to your doctor. Supplements can interact with medications and may have side effects. Self-treating can be risky. Don't rely on supplements as a replacement for a healthy diet and lifestyle. They should be considered as potential additions, not magic bullets.
Acupuncture & Acupressure: Ancient Techniques, Modern Benefits
Acupuncture and acupressure are ancient Traditional Chinese Medicine techniques that are gaining traction in the West for pain management. Acupuncture involves inserting thin needles into specific points on the body to stimulate energy flow and promote healing. Acupressure uses similar points, but instead of needles, it applies pressure with fingers or other tools. Both are believed to influence the nervous system and release endorphins.
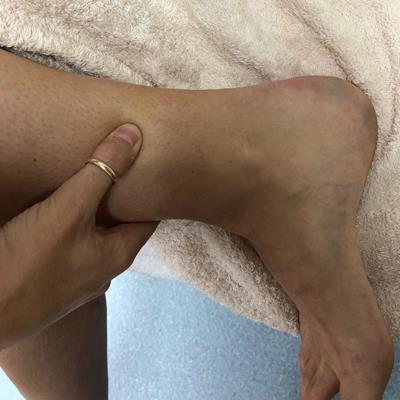
There are specific acupressure points that you can try at home. The Spleen 6 point (located four finger-widths above the inner ankle bone) and the Liver 3 point (between the big toe and second toe) are often recommended for period pain. Applying firm, circular pressure to these points for a few minutes can provide relief. Numerous online resources provide diagrams illustrating these points.
The evidence for acupuncture’s effectiveness is still evolving. Some studies suggest it can reduce period pain, but more research is needed. It’s not a guaranteed solution, and results vary. It’s important to find a qualified and licensed acupuncturist if you’re considering this treatment option.
When to See a Doctor: Red Flags & Next Steps
While many natural remedies can effectively manage period pain, it’s crucial to know when to seek medical attention. Pain that severely interferes with your daily life – making it difficult to work, attend school, or participate in activities you enjoy – is a red flag. Similarly, if over-the-counter pain medications aren’t providing relief, it’s time to see a doctor.
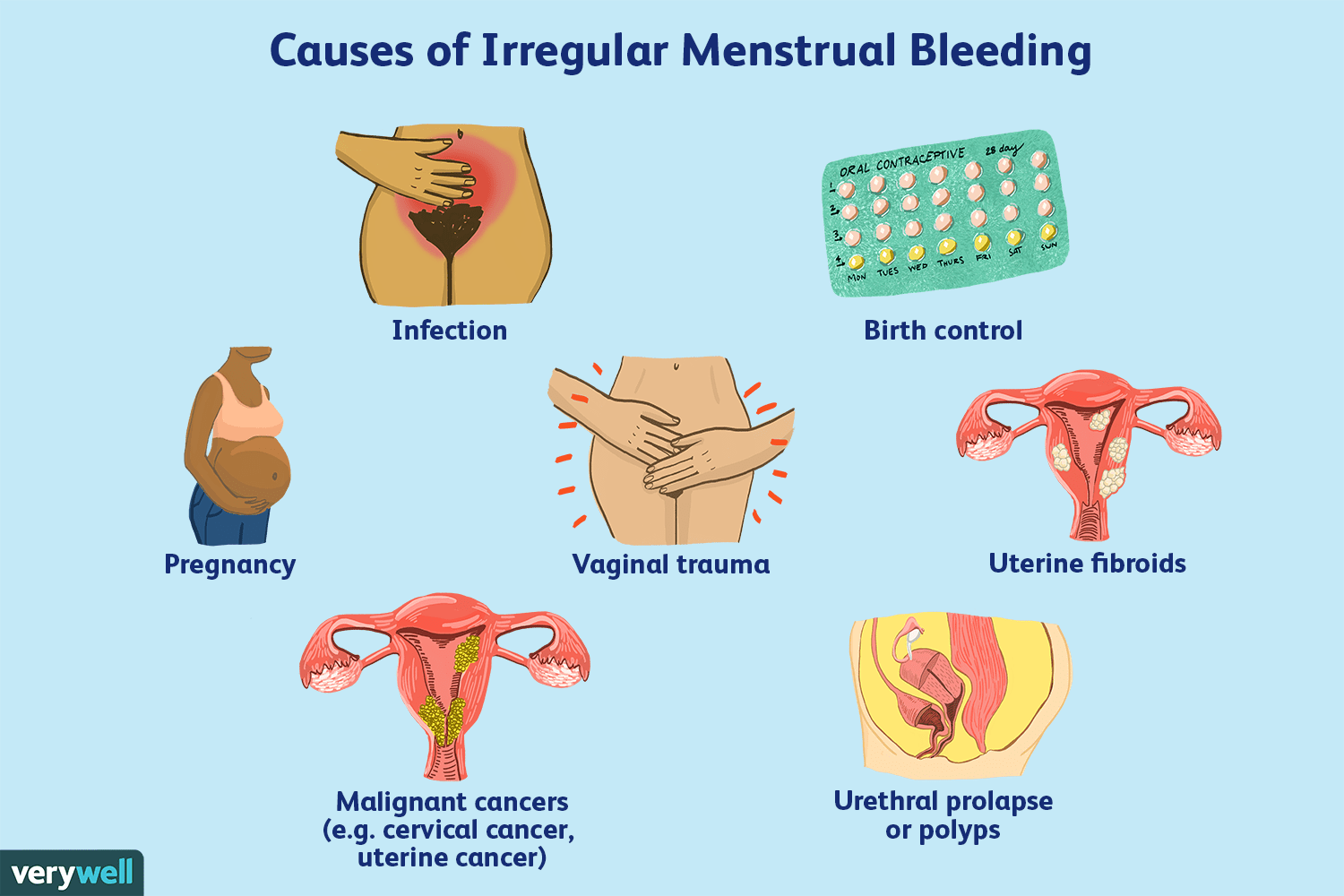
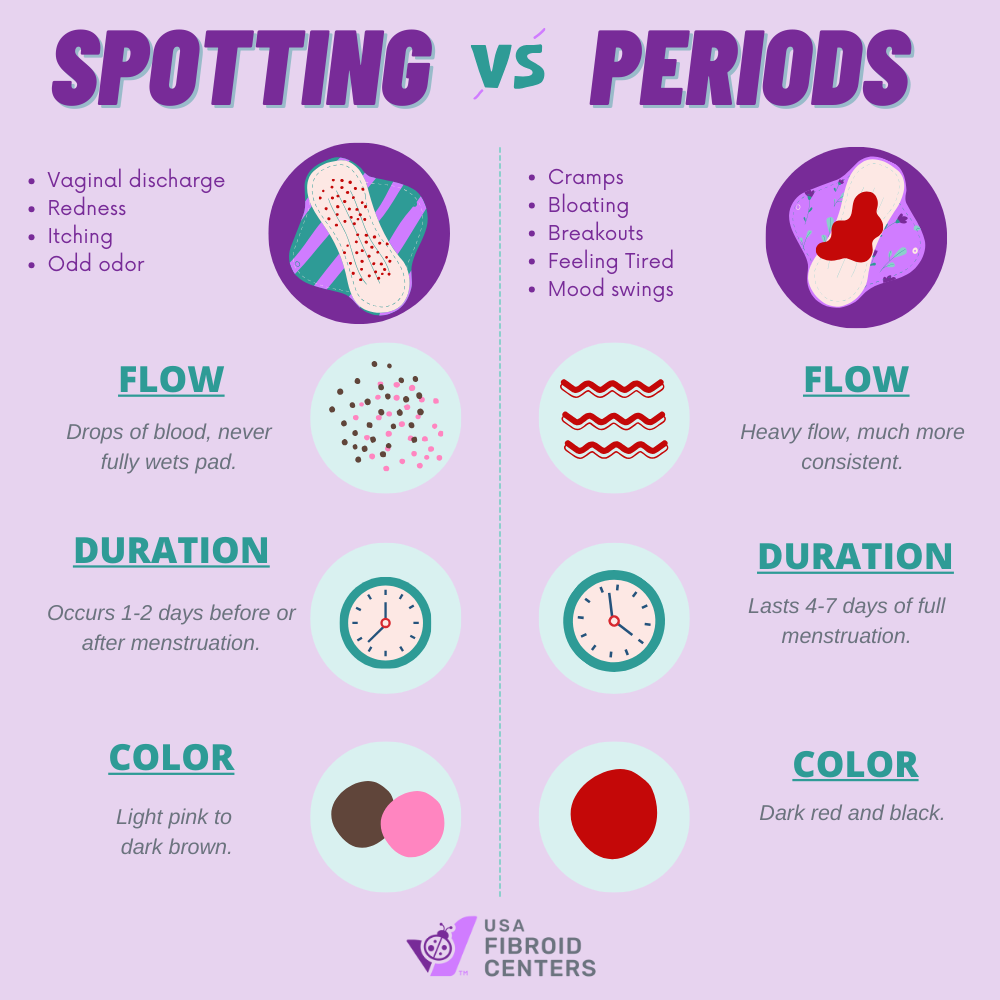
Other warning signs include extremely heavy bleeding (soaking through a pad or tampon every hour for several hours), irregular cycles, pain that lasts longer than your period, or pain accompanied by other symptoms like fever, nausea, vomiting, or diarrhea. These could indicate an underlying medical condition that requires treatment. The Mayo Clinic emphasizes the importance of seeking medical attention for unusually severe or persistent pain (Mayo Clinic, Menstrual cramps, 2024).
During a doctor’s visit, you can expect a discussion of your medical history and symptoms. They may perform a pelvic exam and order tests, such as an ultrasound or blood tests, to rule out underlying conditions. Don't hesitate to advocate for yourself and ask questions. Your health is important, and seeking professional guidance is a sign of strength, not weakness.




No comments yet. Be the first to share your thoughts!