Why Your Period Hurts (Really)
Most people experience some level of discomfort during their periods, but truly debilitating cramps aren't just an unavoidable part of life. The pain stems from prostaglandins, hormone-like substances your body releases to encourage your uterus to contract and shed its lining. These contractions restrict blood flow to the uterine muscle, causing pain. It's similar to what happens when you have a muscle cramp anywhere else in your body, but the location makes it particularly unpleasant.
Inflammation also plays a big role. Prostaglandins don’t just cause contractions; they also contribute to inflammation, which further intensifies the pain. Reduced blood flow means less oxygen is delivered to the uterine muscles, increasing discomfort. It's a cascade of biological events, and understanding them is the first step toward finding relief.
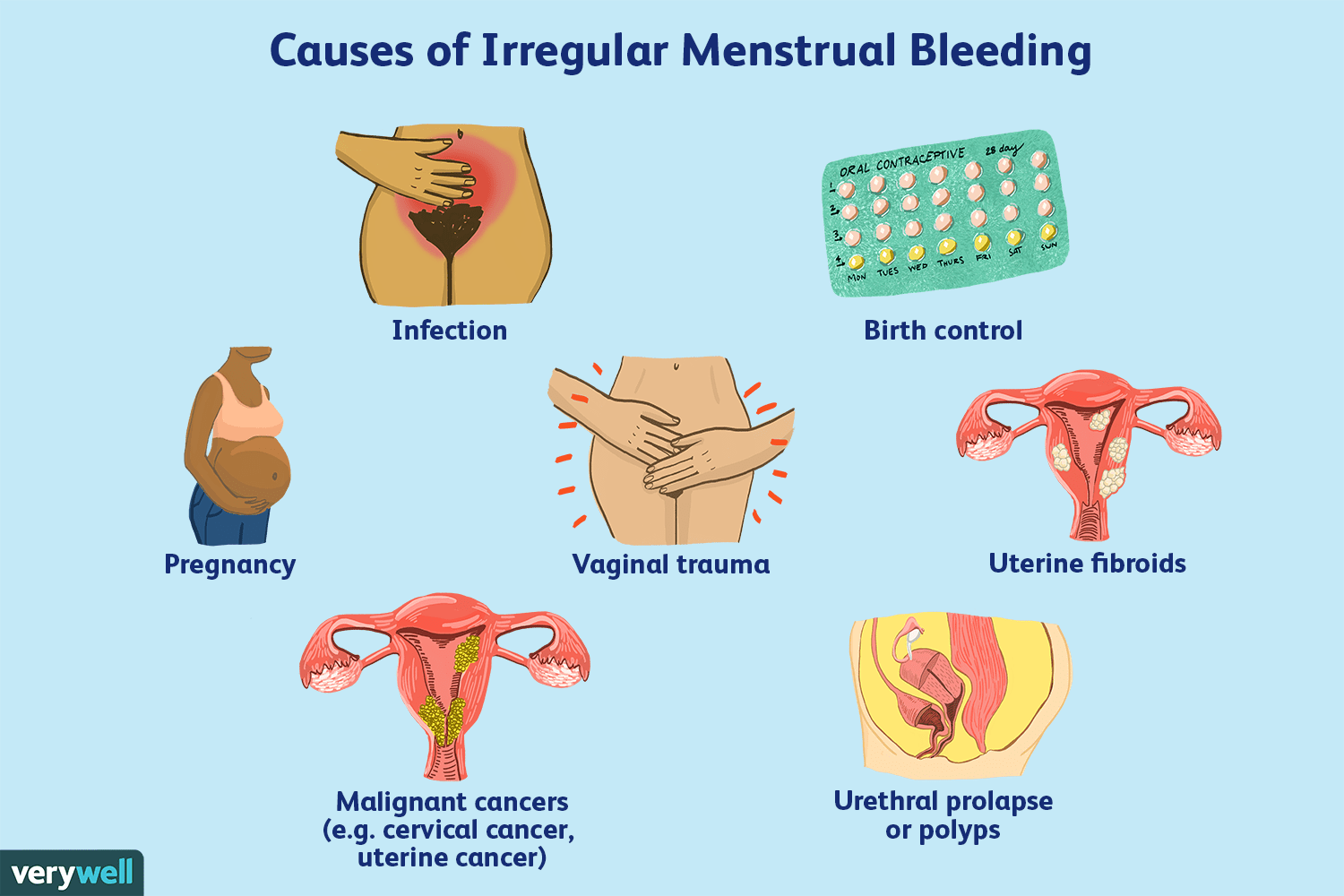
There’s a difference between primary dysmenorrhea – the common cramps most people experience, starting shortly before or during their period – and secondary dysmenorrhea. Secondary dysmenorrhea is caused by an underlying medical condition, like endometriosis, uterine fibroids, or adenomyosis. While this article focuses on natural remedies for primary dysmenorrhea, it’s important to know when your pain might signal something more serious. Don’t just accept intense pain as "normal".

Heat: Your First Line of Defense
Applying heat is one of the oldest and most effective ways to relieve menstrual cramps. Heat works by relaxing the uterine muscles, easing those contractions. It also increases blood flow to the area, delivering much-needed oxygen and reducing pain signals.
You have options: heating pads are a classic, and many now come with adjustable heat settings and automatic shut-off features for safety. Hot water bottles are another reliable choice, though you need to be careful to avoid burns. Warm baths are incredibly soothing, and adhesive heat patches offer discreet, portable relief. The HotSpot reusable heat patch is a good option for use at work.
Safety is important. Never apply heat directly to your skin for extended periods. Always use a cover, like a towel, and avoid falling asleep with a heating pad on. The goal is gentle, consistent warmth, not a burn. Heat is an active intervention that impacts the physiological processes causing your pain.
Movement: Gentle Relief, Big Impact
It might seem counterintuitive when you’re curled up in pain, but gentle movement can actually be incredibly effective for relieving menstrual cramps. Light exercise releases endorphins, natural pain relievers that boost your mood and reduce your perception of pain. It also improves circulation, helping to deliver oxygen to your uterine muscles.
Consider walking, yoga, and gentle stretching. Specific yoga poses like Child’s Pose, Cat-Cow, and Supine Twist can be particularly helpful in releasing tension in your lower back and abdomen. Aim for a moderate intensity walk – something that gets your heart rate up slightly, but doesn’t leave you breathless. Listen to your body.
When you have cramps, exercising might be the last thing you feel like doing. But even 15-20 minutes of gentle movement can make a noticeable difference. Start slowly, and don’t be afraid to modify poses or take breaks when you need them. Find what feels good for your body, not what forces you through a strenuous workout.
- Child’s Pose: Gently stretches the lower back and abdomen.
- Cat-Cow: Improves spinal mobility and releases tension.
- Supine Twist: Gently massages abdominal organs.
Dietary Tweaks: What to Eat (and Skip)
What you eat can significantly impact your period symptoms, including cramps. Focusing on anti-inflammatory foods can help reduce the overall inflammation contributing to your pain. Fatty fish like salmon and tuna are rich in omega-3 fatty acids, which have anti-inflammatory properties. Leafy greens, berries, nuts, and seeds are also good choices.
Conversely, certain foods can worsen inflammation and cramps. Processed foods, sugary drinks, and excessive caffeine should be limited. Alcohol can also exacerbate symptoms. You don't need to overhaul your entire diet, but making small, conscious changes can make a difference.
Magnesium and calcium are two minerals important for menstrual health. Magnesium helps relax muscles, while calcium plays a role in muscle function. Good sources of magnesium include dark chocolate, avocados, and spinach. Calcium is found in dairy products, fortified plant milks, and leafy greens. Incorporate more of these foods into your diet during your period.
Supplements: Beyond the Hype
The supplement aisle can be overwhelming, and it's easy to fall for marketing claims. Let’s look at the evidence for some common supplements used for menstrual cramps. Magnesium has shown some promise in reducing cramps, particularly in women with magnesium deficiency. A 2020 meta-analysis in Pain found a modest benefit. However, high doses can cause digestive upset, so start low and increase gradually.
Calcium, often paired with magnesium, may also help. Vitamin D is important for overall health and may play a role in reducing inflammation, but the evidence specifically for menstrual cramps is limited. Omega-3 fatty acids, found in fish oil supplements, have anti-inflammatory properties and may reduce cramp severity, but more research is needed. Ginger has been traditionally used for menstrual pain, and some studies suggest it can be as effective as ibuprofen, but the results are mixed.
Supplements aren’t a magic bullet. They can be helpful in addition to other lifestyle changes, but they shouldn’t be seen as a replacement for a healthy diet and exercise. Be cautious about taking high doses of any supplement, and always talk to your doctor before starting a new regimen, especially if you have underlying health conditions or are taking other medications. The quality of supplements also varies greatly, so choose reputable brands.
Don't expect instant results. It often takes several cycles to see if a supplement is making a difference. What works for one person may not work for another. Experiment to find what's right for you.
- Magnesium: May reduce cramps, especially with deficiency. Watch for digestive upset.
- Calcium: Often paired with magnesium. Supports muscle function.
- Vitamin D: Important for overall health, limited evidence for cramps.
- Omega-3 Fatty Acids: Anti-inflammatory, may reduce cramp severity.
- Ginger: May be as effective as ibuprofen, but results are mixed.
Comparing Natural Supplements for Menstrual Cramp Relief
| Supplement | Evidence Strength | Typical Dosage | Potential Side Effects | Cost |
|---|---|---|---|---|
| Magnesium | Medium | 200-400mg daily | Diarrhea, nausea, stomach cramps (with high doses) | $ |
| Calcium | Low | 1200mg daily (total intake from diet & supplements) | Constipation, kidney stones (with very high doses) | $ |
| Vitamin D | Low | 600-800 IU daily | Nausea, vomiting, weakness, frequent urination (with very high doses) | $ |
| Omega-3 Fatty Acids | Medium | 1-2 grams of EPA+DHA daily | Fishy aftertaste, gastrointestinal upset, increased bleeding risk (high doses) | $$ |
| Ginger | Medium | 500-2000mg daily (divided doses) | Heartburn, diarrhea, stomach discomfort | $ |
Illustrative comparison based on the article research brief. Verify current pricing, limits, and product details in the official docs before relying on it.
Acupuncture & Acupressure: Ancient Techniques, Modern Support
Acupuncture and acupressure are ancient Traditional Chinese Medicine techniques that involve stimulating specific points on the body to promote healing. Acupuncture uses thin needles, while acupressure uses finger pressure. Both are believed to work by releasing endorphins and improving blood flow.
Research on the effectiveness of acupuncture for menstrual cramps is mixed, but some studies suggest it can provide significant pain relief. A review published in Fertility and Sterility in 2018 found that acupuncture was associated with a reduction in menstrual pain intensity. Acupressure, which you can practice yourself, may also be helpful. Specific acupoints, like SP8 (Spleen 8) and LV8 (Liver 8), are traditionally used for menstrual pain.
Skepticism is understandable
When to See a Doctor
While many natural remedies can effectively manage menstrual cramps, it’s crucial to know when to seek medical attention. If your pain is severe and doesn’t respond to home remedies, it’s time to see a doctor. Heavy bleeding, irregular cycles, or pain between periods are also red flags.
These symptoms could indicate an underlying condition like endometriosis, uterine fibroids, or pelvic inflammatory disease. Getting a diagnosis is essential for appropriate treatment. Don't suffer in silence – your doctor can help determine the cause of your pain and develop a plan to manage it.
Emerging Research: What's on the Horizon?
Research into menstrual pain is ongoing. Scientists are exploring new medications that target prostaglandins and inflammation with greater precision. Non-invasive pain relief techniques, like transcutaneous electrical nerve stimulation (TENS), are also being investigated. TENS uses low-voltage electrical currents to stimulate nerves and block pain signals.
Perhaps most exciting is the increasing focus on understanding the underlying causes of menstrual pain and developing personalized treatment approaches. As we. It’s a hopeful time for menstrual health.




No comments yet. Be the first to share your thoughts!