Your Period in Flux: What’s Happening?
Have you noticed your period acting different lately? You're not alone. Many people are discussing changes to their cycles, and it's understandable to feel anxious when something shifts. Menstrual cycles aren't set in stone; they naturally fluctuate throughout life, responding to internal and external influences.
These changes aren’t always a cause for concern; sometimes they’re normal adjustments. But significant or persistent shifts deserve attention. Understanding what’s typical and what might signal a need to chat with a healthcare provider is key to staying on top of your menstrual health. We've drawn on information from the Mayo Clinic and the National Center for Biotechnology Information (NCBI).
This is about empowering you with knowledge. Knowing what to expect—and what isn't normal for you—can make all the difference in advocating for your well-being.

The Usual Suspects: Common Cycle Variations
Everyday factors can throw your cycle off. Stress is a huge one. When you’re constantly stressed, your body releases cortisol, which can disrupt the delicate hormonal balance needed for a regular cycle. Your body is prioritizing survival mode over reproduction.
Weight fluctuations can also play a role. Significant weight loss or gain can impact the hypothalamic-pituitary-ovarian (HPO) axis – the communication network between your brain and ovaries, which is essential for regulating your period. That intense training for the marathon? It might be why your period went missing for a month, as your body dialed down reproductive function to conserve energy.
Dietary changes and exercise routines also matter. A sudden shift to a restrictive diet or a dramatic increase in physical activity can disrupt hormonal balance. Even travel can cause temporary changes due to jet lag and routine shifts. These disruptions are usually temporary, and your cycle should return to normal once the stressor is removed. But if changes persist, further investigation is needed.
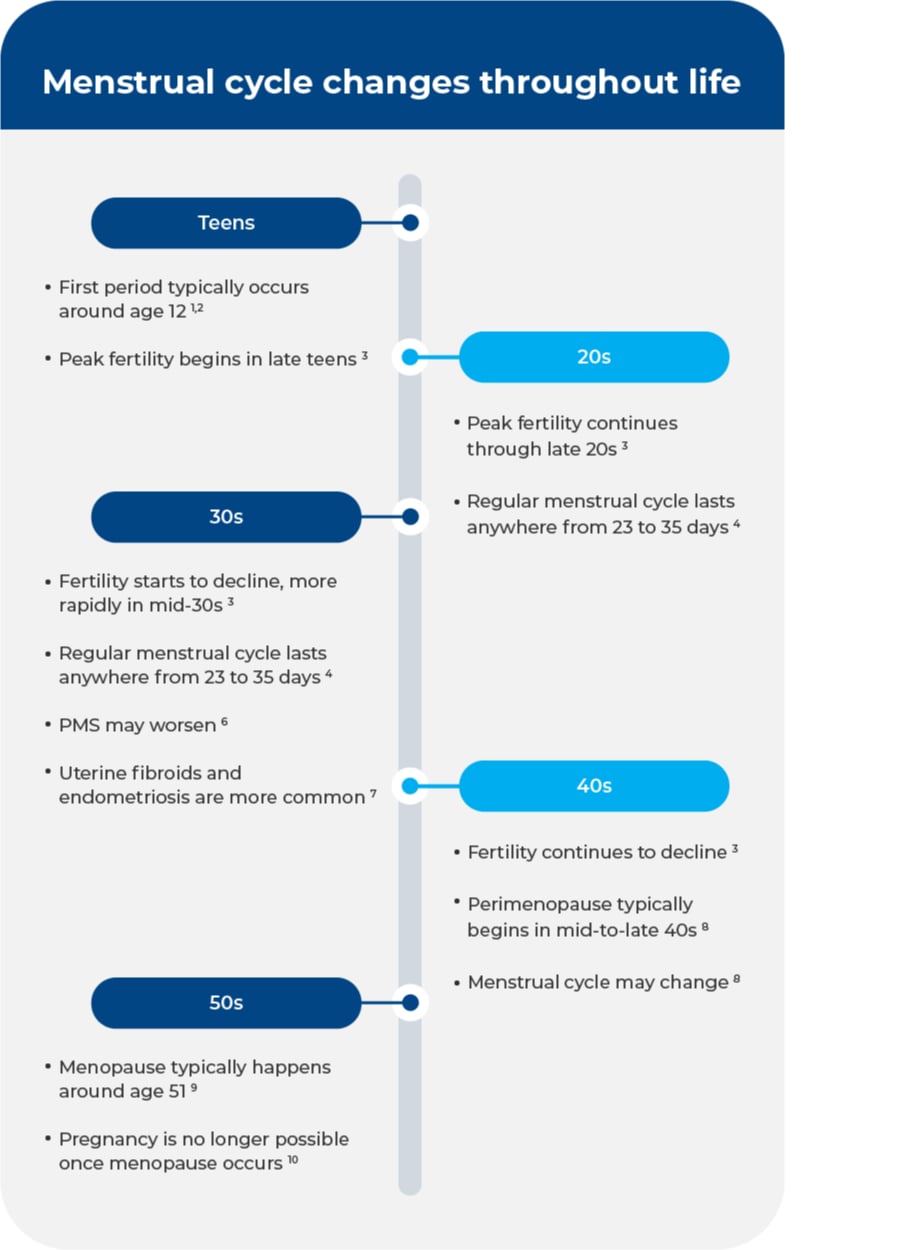
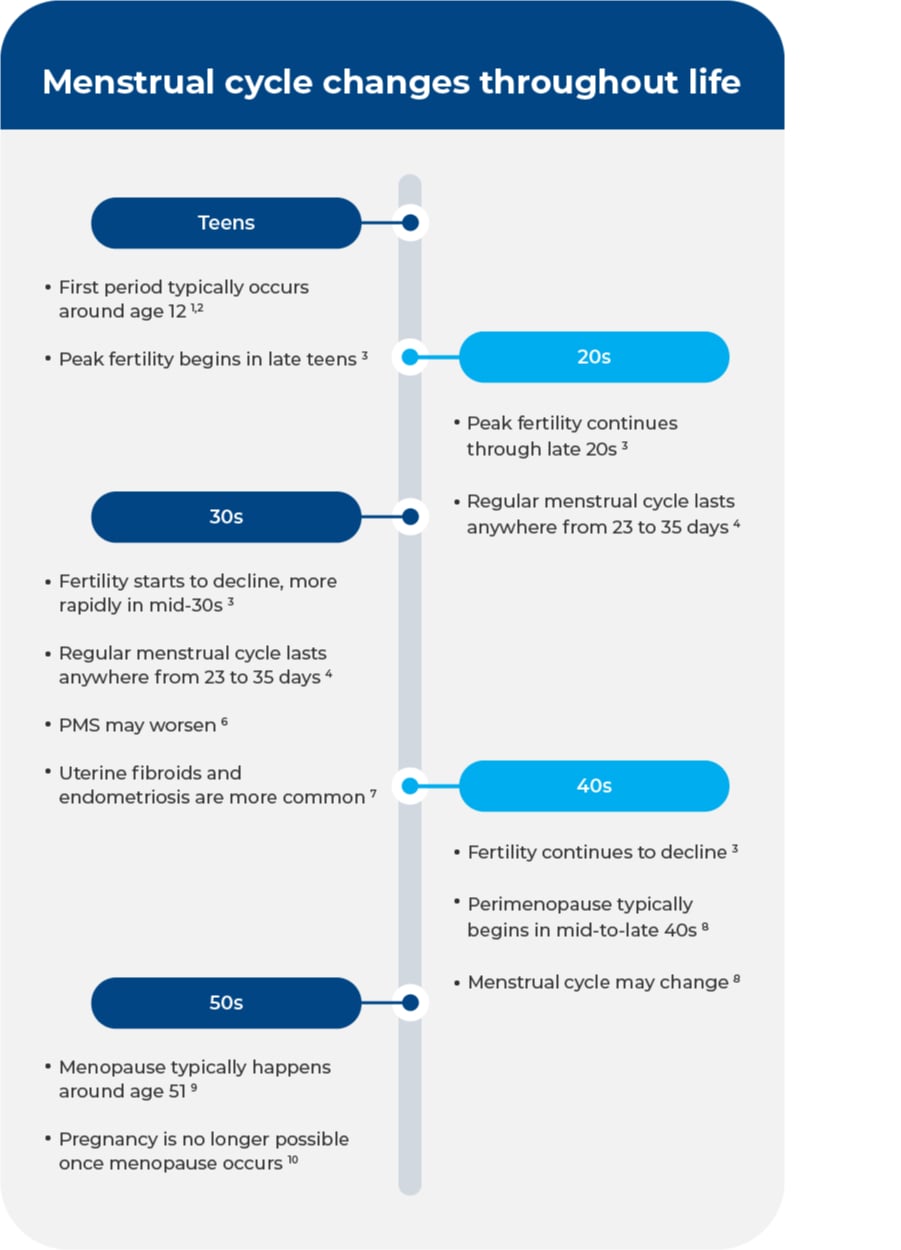
Age and Stage: Cycle Shifts Through Life
Menstrual cycles change as we age, and that's normal. When you first get your period (menarche), cycles are often irregular for the first few years as your body establishes a consistent hormonal pattern. It can take several years for cycles to become more predictable.
During your reproductive years, cycles typically become more regular, but variations still occur. The average cycle is 28 days, but anything between 21 and 35 days is considered normal. Cycles can still be influenced by stress, diet, exercise, and other factors.
As you approach perimenopause, the years leading up to menopause, cycles become increasingly irregular again due to declining ovarian function and fluctuating hormone levels. You might experience changes in cycle length, flow, and new symptoms like hot flashes or sleep disturbances. The NCBI explains this transition is a natural part of aging, but can be managed with your doctor's support.
Spotting Beyond Your Period: What Does It Mean?
Spotting – light bleeding that isn't a full period – can be confusing. It differs from a typical period in amount and duration. A period usually lasts several days with a heavier flow, while spotting is lighter and shorter-lived.
Many factors can cause spotting. Hormonal imbalances, often linked to starting or stopping birth control, are common. Changes in birth control methods, like switching from pills to an IUD, can also cause temporary spotting. Sometimes, spotting can be a sign of sexually transmitted infections (STIs), so it’s important to rule those out if you're sexually active.
Less commonly, spotting can be caused by non-cancerous growths in the uterus, such as polyps or fibroids. While usually harmless, these growths can sometimes cause irregular bleeding. In rare cases, spotting could be a sign of a more serious issue, so pay attention to patterns and seek medical advice if you’re concerned.
- Hormonal imbalances
- Birth control changes
- STIs
- Uterine polyps/fibroids
- Less common, more serious causes
When Changes Signal Something More
Know when a change in your period warrants a doctor's visit. Suddenly very heavy bleeding – soaking through a pad or tampon every hour for several hours – is a red flag. Periods lasting longer than usual, exceeding seven days, also need to be checked out.
Complete absence of periods for three months or more (when not pregnant) is another sign something might be amiss. Severe pain that doesn't respond to over-the-counter pain medication is concerning. Bleeding between periods that is new or worsening, or any spotting after menopause, should be investigated promptly.
This is not medical advice. If you’re experiencing any of these symptoms, please schedule an appointment with your doctor to discuss your concerns and get a proper diagnosis.
Underlying Conditions: Potential Connections
Changes in your menstrual cycle can sometimes be a symptom of an underlying medical condition. Polycystic ovary syndrome (PCOS), for example, is a hormonal disorder that can cause irregular periods, heavy bleeding, and other symptoms. Endometriosis, a condition where tissue similar to the lining of the uterus grows outside the uterus, can also lead to painful and irregular periods.
Thyroid disorders – both hypothyroidism (underactive thyroid
If you're experiencing significant cycle changes, it's important to discuss these potential connections with your doctor. Early diagnosis and treatment of underlying conditions can help manage symptoms and improve your overall health. You can find more information on these conditions from organizations like the Mayo Clinic and the Cleveland Clinic.
Tracking for Insight: Knowing Your Baseline
One of the best things you can do for your menstrual health is to start tracking your cycle. This helps you understand what's normal for you and identify any deviations from your baseline. There are several methods you can use. Calendar tracking is a simple way to mark the start and end dates of your periods.
Period tracking apps, like Periuod, make it easy to log your cycle, symptoms, and other relevant information. Basal body temperature (BBT) charting involves taking your temperature every morning before getting out of bed to identify subtle shifts that can indicate ovulation. Cervical mucus monitoring involves observing changes in the consistency of your cervical mucus throughout your cycle.
By tracking your cycle over time, you can gain valuable insights into your hormonal patterns and identify any potential problems. Periuod offers a range of tracking features designed to help you stay informed and proactive about your menstrual health.
Comparing Cycle Tracking Methods
| Ease of Use | Cost | Accuracy | Information Provided |
|---|---|---|---|
| Very Easy | Low | Basic | Cycle Length |
| Easy | Low | Moderate | Possible Ovulation |
| Moderate | Low to Moderate | Better for identifying ovulation | Basal Body Temperature shifts |
| Moderate | Low | Moderate to High | Fertility window, cervical changes |
| Difficult | Moderate to High | Highest | Hormonal fluctuations, cycle irregularities |
| Easy | Moderate | Moderate | Comprehensive cycle data, pattern recognition |
Qualitative comparison based on the article research brief. Confirm current product details in the official docs before making implementation choices.
Navigating the Conversation with Your Doctor
Talking to your doctor about changes in your period can feel daunting, but it’s essential for getting the care you need. Before your appointment, keep a detailed cycle diary, noting the start and end dates of your periods, the amount of bleeding, and any symptoms you’re experiencing.
Write down any specific concerns you have, and be prepared to answer questions about your lifestyle factors—stress levels, diet, exercise, and any medications you’re taking. Don’t hesitate to advocate for yourself and ask questions until you feel comfortable and understood.
Remember, your doctor is there to help. Providing them with accurate and detailed information will allow them to make the best possible assessment and recommend appropriate treatment options. Don't downplay your symptoms or feel embarrassed to discuss intimate details—your health is worth it.



No comments yet. Be the first to share your thoughts!