Understanding spotting
Spotting between periods is common and can be alarming, but it's not always a sign of something serious. This article covers common causes, emerging treatment approaches, and when to seek medical advice.
Spotting differs from a light period. It's a small amount of blood, appearing as streaks or drops. We'll discuss what causes these menstrual cycle changes and how to manage them. Research into the vaginal microbiome's role in menstrual health is influencing new treatments.
Personalized care is becoming more common in health, including managing period symptoms like spotting. Understanding the root cause is key, with more tools and treatments available than ever. Knowing what's happening in your body helps you feel more in control.
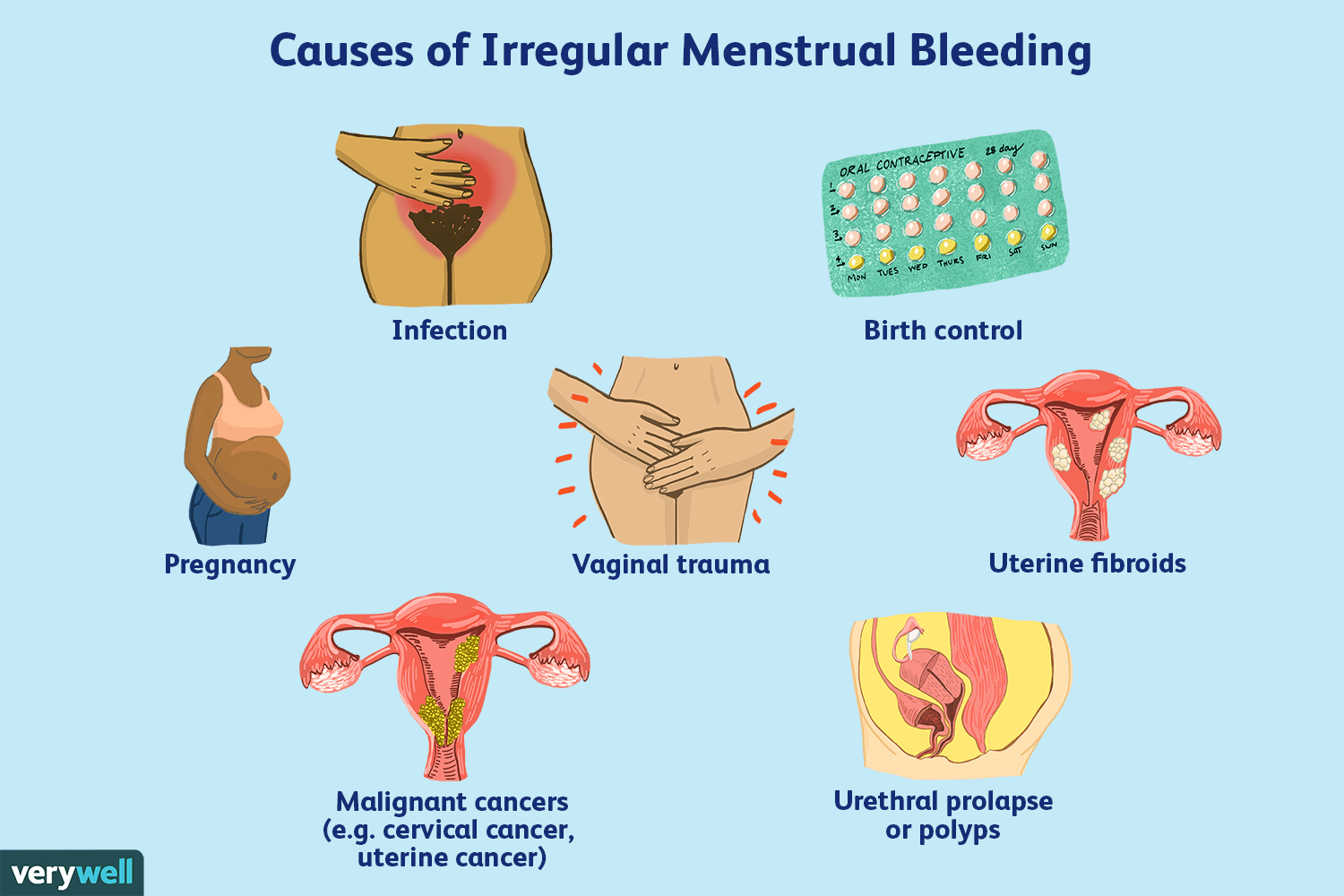
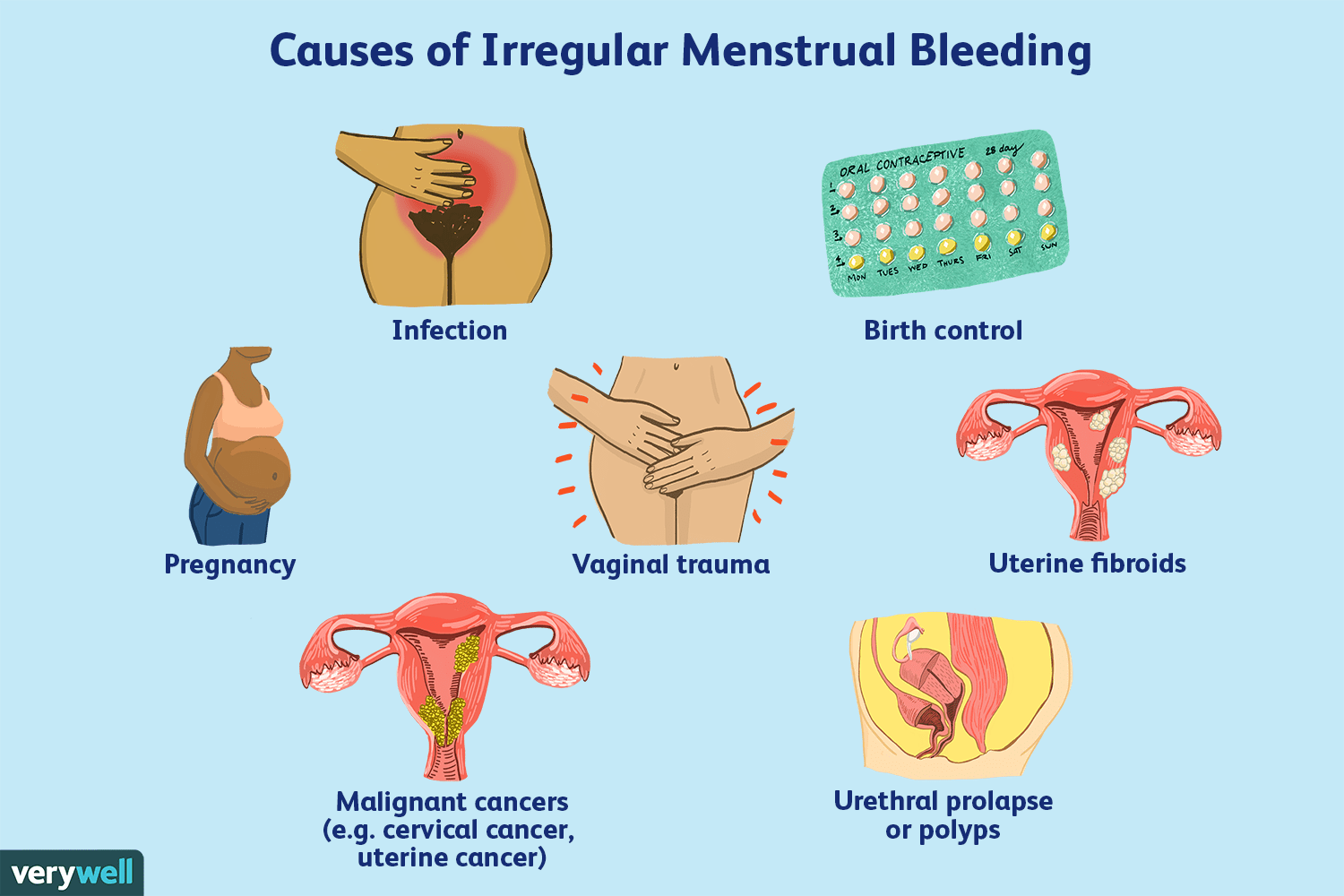
Common causes
Hormonal birth control is a frequent culprit behind spotting. Starting, stopping, or switching methods—pills, patches, rings, IUDs—can all disrupt your cycle and cause unexpected bleeding. This is because these methods work by manipulating hormone levels, and it takes time for your body to adjust to those changes.
Ovulation spotting is another common cause, often referred to as mittelschmerz. This happens when the egg is released from the ovary, and the follicle ruptures. The resulting hormonal shift and slight irritation can lead to a small amount of bleeding or spotting. Essentia Health notes that spotting before your period can often be related to these hormonal fluctuations.
Stress also plays a significant role. High cortisol levels from stress can interfere with the menstrual cycle, leading to irregular bleeding or spotting. This shows how interconnected physical and emotional health are. Changes in routine or travel can also contribute.
Finally, early pregnancy can sometimes cause spotting, often mistaken for a period. This is known as implantation bleeding and happens when the fertilized egg attaches to the uterine lining. It's usually lighter than a regular period and doesn’t last as long, but it’s important to confirm pregnancy with a test if you suspect this might be the cause.
Hormonal Shifts & Life Stages
Hormonal fluctuations aren't limited to birth control and ovulation. Throughout life, our hormone levels naturally shift, and these changes can often lead to spotting. Perimenopause, the transition period before menopause, is a prime example. As estrogen levels decline, cycles become irregular, and spotting between periods is very common.
Polycystic Ovary Syndrome (PCOS) is another condition that can cause spotting. PCOS involves an imbalance of reproductive hormones, leading to irregular periods and ovulation. This irregularity can manifest as spotting between periods. It’s often accompanied by other symptoms like acne, hirsutism (excess hair growth), and weight gain.
Thyroid issues—both hypothyroidism (underactive thyroid) and hyperthyroidism (overactive thyroid)—can also disrupt the menstrual cycle. Thyroid hormones play a crucial role in regulating metabolism, which impacts hormone production. An imbalanced thyroid can lead to irregular periods and spotting. It's important to get a thyroid panel done if you're experiencing these symptoms.
Lifestyle factors also contribute. Extreme exercise or significant weight changes can disrupt hormone balance and cause spotting, especially in athletes or those drastically altering their diet. The body needs hormonal stability to function optimally. Recognizing these patterns helps in understanding what's happening.
2026: Emerging Treatment Approaches
Spotting treatment is becoming increasingly personalized. In 2026, personalized hormone therapy, guided by cycle tracking apps and at-home hormone tests, is rising. These tools help individuals monitor hormone levels and adjust therapy with their doctor.
The vaginal microbiome is receiving attention. Research indicates that bacterial imbalance can contribute to menstrual irregularities, including spotting. Microbiome-targeted therapies, like probiotics and vaginal suppositories to restore bacterial balance, are being explored. These aim to regulate the menstrual cycle by addressing the microbial environment.
For PCOS-related spotting, researchers are investigating non-hormonal treatments to regulate the menstrual cycle without the side effects of traditional hormone therapy. These include medications that improve insulin sensitivity and reduce inflammation. Many are still in clinical trials, but early results are promising.
Advancements in diagnostic tools are also being made. More sophisticated hormone tests are becoming available for precise assessment of hormonal imbalances. This detail is crucial for tailoring treatment to individual needs, moving away from a one-size-fits-all approach towards a targeted strategy.
When Spotting Signals a Doctor's Visit
While spotting is often harmless, some situations warrant a doctor's visit. Heavy spotting, defined as soaking through a pad every hour for several hours, is a red flag and could indicate a serious underlying issue like uterine fibroids or endometriosis.
Spotting with severe pain is also concerning. This could signal pelvic inflammatory disease (PID), ectopic pregnancy, or other serious conditions. Pain that is debilitating or doesn't respond to over-the-counter pain relievers needs evaluation by a healthcare professional.
Spotting after menopause is never normal and requires investigation. It could signal endometrial cancer or other serious health problems. Spotting with fever or dizziness also requires immediate medical attention, as these symptoms could indicate an infection or acute illness.
Finally, report any sudden changes in spotting patterns to your doctor. This includes a significant increase in bleeding, a change in blood color, or blood clots. These changes could indicate a new or worsening condition.
Diagnostic Tools: What to Expect
If your doctor suspects an underlying cause for spotting, they may recommend diagnostic tests. A pelvic exam is a standard first step to visually inspect reproductive organs for abnormalities.
Blood tests are often ordered to check hormone levels, complete blood count (to rule out anemia), and thyroid function. These tests help identify hormonal imbalances or other medical conditions. Your doctor may also check for pregnancy.
An ultrasound can provide a detailed image of your uterus, ovaries, and fallopian tubes. This can help identify fibroids, polyps, cysts, or other structural abnormalities. There are two types of ultrasounds: transabdominal (done on the abdomen) and transvaginal (done inside the vagina for a clearer image).
In some cases, an endometrial biopsy may be necessary. This involves taking a small tissue sample from the uterine lining to check for cancer or abnormalities. It's invasive but provides valuable information. These tests aim to identify the root cause of spotting and guide treatment decisions.
Navigating the Conversation with Your Doctor
Talking to your doctor about spotting can feel uncomfortable, but it's essential for getting care. Before your appointment, track your cycles and spotting patterns, noting the dates, duration, and amount of bleeding. This information is invaluable to your doctor.
Don’t hesitate to ask questions, such as: “What are my hormone levels?”, “What are my treatment options?”, and “What are the potential risks and benefits of each treatment?” Be honest and open about your symptoms and concerns.
You are your own best advocate. Seek a second opinion if you're not satisfied with your doctor’s recommendations. Feeling comfortable and confident in your care is important. Taking an active role in your health empowers informed decisions.
Spotting & Periuod Products
Managing unexpected spotting can be easier with the right products. Periuod period underwear offers a comfortable and discreet solution for light bleeding, providing peace of mind throughout the day. Menstrual cups are another excellent option, offering a leak-proof and eco-friendly alternative to pads and tampons.
Of course, period pads remain a reliable choice for managing spotting. Choose pads that are specifically designed for light flow to ensure maximum comfort and protection. Ultimately, the best product for you will depend on your individual preferences and the amount of spotting you’re experiencing.





No comments yet. Be the first to share your thoughts!